By Jeannette Freeman, leader of API of Southeast Texas

Editor’s Note: Attachment Parenting International does not advocate unassisted birth of any sort. We believe the safest birthing environment for every baby, whether at home or in a hospital or birthing center, is with assistance from a midwife, obstetrician, or another accredited birthing assistant. The following article has been published to give this mother a voice in telling her birth story only, without any endorsement of her decisions made regarding her child’s birth.
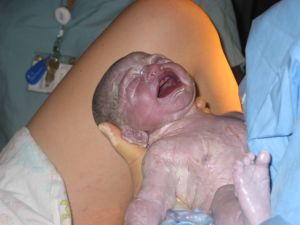
Luke Elliot was born Friday, Sept. 21, at 5:43 p.m., shortly before sunset and the beginning of the Day of Atonement (Yom Kippur). My “due date” had been the previous Saturday, and I really wanted him to be born before the next Sabbath, as I was tired of everyone at church being surprised that he hadn’t arrived yet.
My original due date had been off by two months, and some of the mother hens of the congregation, namely those who birthed in the 1950s and ’60s, were more than a little anxious about my unassisted pregnancy and planned unassisted birth. It had gotten to the point when my husband, Mark, and I decided to visit an obstetrician to calm everyone’s nerves. The doctor refused to touch me unless I was willing to submit to a vaginal exam and whatever else he deemed necessary. I refused.
The morning of Luke’s birth, Mark, my two-year-old daughter Audrey, and I spent over an hour picking up branches and leaves from our front yard after Hurricane Humberto our first hurricane experience had hit the week previous. After I put Audrey down for her nap, I commented to Mark, “We may have started something,” referring to the yard work and my now-present uterine contractions. When Audrey awoke at 2:45 p.m., my labor became active. There was no stopping now!
It was a rather surreal labor, as I chose different positions, consulted two different birthing books, gave instructions to my husband, and practiced a variety of vocalizations to figure out what did and did not work for me, mindful than some noises might startle my daughter.
Our bathroom truly a one-person room became my center of command. For awhile, I labored on the toilet, leaning on a pillow resting on a TV tray table. For awhile, I labored on my hands and knees. My butt was in the bathroom and my torso in the hallway. Between contractions, I was leaning forward on two large couch pillows with my butt up in the air to slow progress down a bit. This was entirely different from Audrey’s labor that lasted so long I was literally out of energy before it was over. It was during this period that Audrey insisted that her father get her a pillow of her own to lie on. Now, when I leaned forward on my pillows during contractions, she did too. I wish I had a picture of that!
I consulted a book to determine if I had entered the transition stage yet. I had. I then read that after transition, there was often a release of endorphins. I felt that rush, than had two more contractions that felt like they were still part of transition before my body moved onto the pushing stage. During the pushing stage, I hung on the bathroom door.
A little bit into the pushing stage, I reached into my vagina to feel Luke’s head. This is something I had never considered doing, but it was exhilarating to touch the little person I had been waiting for months to see.
By this time, my husband and daughter were sitting outside the bathroom door and watching. A few more pushes and Luke’s head crowned. I took my time, knowing that he would come out eventually and that I didn’t want to tear. Soon, he was part way out. I got a hold of him and realized I could catch him myself, so I did. I was ecstatic. I held my boy for a few long moments and then exclaimed, “We did it!”
When I looked at the umbilical cord, it was already white and ready to cut. This was a good thing, as it was rather short. I suspected it would be, as it was with Audrey, and it was rather awkward to hold Luke. My husband did the honors. I balked at the smell of the rubbing alcohol he used to clean his pocketknife. It was offensive to my senses and out of place.
Mmy boy’s head smelled aseptic. It wasn’t a hospital-like, chemically created aseptic smell but a natural cleanness from his time in the womb. It surprised me until I thought about how the womb was indeed a sterile place.
I sat on the floor in the mess for a few minutes and then crawled into the tub while my husband cleaned up. Then, my husband took Luke and Audrey into the library. I ended up birthing the placenta on the toilet. I knew it was coming and I tried to get to the tub. I wanted to check the placenta to make sure it was complete. I did fish it out of the toilet later and put it in a big bowl. I looked at it later but gave up trying to figure out if it was all there. Instead, I put it in a bag to send out with the trash.
Less than an hour after Luke’s birth, I was standing in my shower thinking, “Wow! This is great. Showering in my own shower. Never leaving home to birth my own baby. This is the way to do it. So much more relaxed and peaceful than the hospital.”
Audrey had big plans for her new brother. She had Dad read a book to him, and brought him a block to play with and a pair of her shoes to wear. Mark enjoyed this time of the three of them bonding while I cleaned myself up.
I have no intention of leaving my home to birth again. It was an amazingly empowering event that, three months later, I still ponder with awe.
I began my journey towards an unhindered birth with the belief that my Maker created my body to birth and that He created it perfectly. Planning an unhindered birth was my way of “putting my money where my mouth was.” I’m glad I did.