By Connie Banack, CCCE, CPD, CLD, reprinted with permission from International Cesarean Awareness Network, © ICAN-online.org
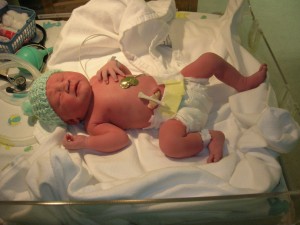
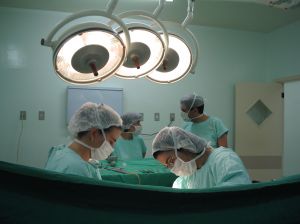 Family-centered birth is used to describe a birth that is more family oriented, allowing the new family to experience their birth more fully. Many believe that this cannot apply to a surgical procedure. This is not true. Even with a Cesarean surgery, you can have a family-centered birth if you know your options and choose to apply them. Some of the options will be the same as for a vaginal birth. You may have to work harder to have a family-centered birth in the event of surgery, but planning ahead — even if you don’t foresee a Cesarean — can go a long way. Make a birth plan! They won’t know what is important to you unless you let them know, and a birth plan is actually a legal contract as it is providing your wishes in a document provided to your birth team.
Family-centered birth is used to describe a birth that is more family oriented, allowing the new family to experience their birth more fully. Many believe that this cannot apply to a surgical procedure. This is not true. Even with a Cesarean surgery, you can have a family-centered birth if you know your options and choose to apply them. Some of the options will be the same as for a vaginal birth. You may have to work harder to have a family-centered birth in the event of surgery, but planning ahead — even if you don’t foresee a Cesarean — can go a long way. Make a birth plan! They won’t know what is important to you unless you let them know, and a birth plan is actually a legal contract as it is providing your wishes in a document provided to your birth team.
Very few women would choose a Cesarean for their birth experience. However, it is important that every pregnant woman is aware of the procedures that surround a Cesarean section. This will give those who do birth by this process more choices and hopefully less fear.
A Word about Doulas
The continuous support of a doula has been found in numerous scientific trials to positively affect obstetric outcomes and the women’s satisfaction with their birth experiences. Many women and couples choose to have a doula because they want and need this extra assistance. During labor, an intense bond develops between the doula and the couple, and if a Cesarean becomes necessary, it is very distressing for the woman to have to choose only one person to be with her. Mothers will hire doulas even during a scheduled Cesarean birth to provide the consistent professional support a doula provides.
A 2001 article by Penny Simkin, “Doulas at Cesarean Birth,” details the benefits of a doula during a Cesarean, which include:
- Doulas are familiar with Cesareans and do not find them upsetting.
- The doula’s familiar presence can calm and reassure the mother who is likely to be very frightened and worried.
- The doula can reassure the partner, who is also likely to be worried and frightened.
- The doula can explain what is happening.
- Once the baby is born, the partner usually goes to see the baby, leaving the mother’s side. The doula remains with the mother, tells her what the baby is doing, and helps the mother feel less alone.
- The doula goes to recovery with the mother. If the partner has gone to the nursery with the baby, the mother still has a support person with her.
- The doula does not get in the way or behave inappropriately.
Check with your doctor to see if your doula is allowed into the operating room and recovery to support you.
Birth Plan Preparation
In preparing a birth plan, each point needs to be discussed with your caregiver, even if he may not be at your birth. He will be able to tell you if what you would like is an option with him or at the hospital you have chosen. Start early and discuss a few points each prenatal visit rather than trying to cover every point in one or two visits. This will help you in providing more time for questions about each point and reduce confusion for both you and your caregiver.
Communication is vital in learning about philosophy, options, and rapport. A good way to communicate with your caregiver in putting together a birth plan that will be read and followed is through the “Who’s the Boss?” Method:
- Acknowledge provider’s expertise
- Add personal information
- Listen and consider
- Summarize
- Respond in appreciative and authoritative mode.
Example:
- You: One of my friends was telling me about avoiding post-operative pain medications just after her baby was born, which made her fall asleep, and I wanted to get your professional opinion on the subject.
- Doctor: Routinely, a pain medication is given to you after the baby is born to help you relax during the long suturing process, which can take up to an hour. It can make you sleepy or even relax you enough to put you to sleep. You can then wake up refreshed when you meet your new baby.
- You: Is it possible to ask not to have this given?
- Doctor: Absolutely.
- You: OK. Thank you for discussing that with me. Now I understand, and I’ll think about what you said before I decide.
When writing your plan, start by introducing yourself through a prologue. This provides a familiar base on which to build a rapport with your nurses and attending caregiver. This is followed by your wishes, which have been discussed with your doctor prior to your birth. Point form is the most efficient way to list these, as you don’t want your birth team to become mired in your plan looking for a lost point. Wording is crucial in a birth plan. It can make all the difference between a supportive or hostile atmosphere during your birth. Yet it is also a legal document.
“The language ‘I do not consent’ may sound harsh but, in fact, is the only statement that has clear legal power so I encourage you to use it for things that you feel strongly about,” emphasizes Gretchen Humphries, editor of BirthTruth.org. “If someone does something to you after you state that you do not consent to it, legally they have committed assault and battery on you. Hospitals are well aware of this, but they assume you are not.”
Make your birth plan short, preferably one page long. Include only those points most important to you. Providing two plans, one for birth and one for your new baby, is an excellent way to ensure that both you and your baby are cared for as you wish. The birth plan stays with you, and the newborn plan goes with your baby if he not able to stay with you. Have several copies with you and give it to everyone involved in your Cesarean. And finally, after you have finished discussing the points with your caregiver, consider having him sign it. This helps ensure that it will be read and followed during your birth.
Basics of a Family-Centered Cesarean Birth Plan
- Prologue — Most nurses and doctors appreciate a prologue to a birth plan. A prologue introduces you to your birth team and can give insight into the choices you have made in the plan itself. For instance, parents who have had a former general anesthesia Cesarean experience could include this in the birth plan as an explanation as to why they are choosing an epidural for this birth.
Example:
We understand that there are times when a Cesarean delivery is in the best interests of the mother and infant. We also understand that Cesarean delivery, as a surgical procedure, is common and even routine in most maternity centers. However, we would ask that the staff respect that this individual surgery is a unique and never-to-be-repeated event in the life of our family. For us, it is neither common nor routine, but rather is an event that will have effects lasting a lifetime. We have already experienced the Cesarean delivery of our sons and, because of that, have certain requests and requirements to be taken into account.
- Pre-operative Preparation — If an elective Cesarean is necessary, then you should request that you be able to begin labor naturally before the Cesarean is done. That is, you do not want a date and time preset; you wish for your baby to decide the day on which it is ready to be born to avoid any problems with prematurity and for both of you to reap the benefits of your hormones. It is also important for your benefit in both recovery and in establishing your breast milk. Labor signals your body to start producing breast milk about two to three days after your baby is born and this is thwarted when baby is removed surgically without labor, often prolonging the production of milk by several days. If a scheduled Cesarean must be performed, then you should request preoperative blood work and tests to be done on an outpatient basis, and hospital admission on the day of the birth not the night before. There are several preparation procedures that are done before you enter the operating room such as establishing an I.V. and giving a bolus of I.V. fluid, placing the epidural catheter and ensuring adequate anesthesia, inserting a urinary catheter, checking of vitals (blood pressure, heart rate, temperature), and checking fetal heart tones. There is no reason why you cannot have your partner and others there to comfort and support you during any of them. One procedure specifically, inserting the urinary catheter, can be quite uncomfortable and many mothers recommend delaying the insertion until after the epidural or intrathecal is in place.
Example:
I do not consent to placement of a urinary catheter until after regional anesthesia is in place, unless it has been discussed with me in advance.
- Anesthesia — Women have three options for anesthetic during a Cesarean section: general anesthesia (mom is unconscious), epidural anesthesia, and intrathecal anesthesia (with both of the latter, mom is awake for the delivery). Please research each option, both for availability and benefits and risks of each to find which is right for you. What many women do not realize if they are awake is that medications are often given before, during, or just after the baby is born to relax the mother, but the postoperative medication especially often puts the mother to sleep. You will need to decide if you want this or not and include it in your birth plan if you want to avoid further pain medications during or after the surgery.
Example:
I do not consent to any pre-, peri-, or postoperative medication without prior verbal consent from myself, or my spouse if I am incapacitated. I wish to discuss the complete anesthesia protocol with the anesthesiologist prior to any medication administration. I desire postoperative analgesia to be administered via epidural before any use of systemic analgesics, sedatives, or tranquilizers. I have used this protocol in the past and was pleased with the results.
- During Surgery — It is the anesthesiologist who makes the decisions in the operating room. It is important that he reviews a copy of your birth plan and discusses it with you prior to your birth. Ensure you include in your birth plan who you would like to attend during and after your birth in the operating room. Some anesthesiologists allow only one person with you in the operating room; others allow two or more. Find out what your options are and prepare accordingly. If only one is allowed, one alternative may be having your partner be with you until the baby checks are completed and then have your doula or another support person come in when your partner leaves with baby, assuming baby is moving to the nursery. Routinely, your hands are strapped down to prevent tangling of the various cords to the medical equipment that is monitoring you and to prevent your arms from falling off the narrow boards they are placed on. You can ask to not have your hands strapped down, so as to better receive your baby when he is brought to you. Would you, and your partner, like to view the actual birth? Then make sure your obstetrician realizes this. Explain you would like the option of viewing the birth, either by lowering the screen or by positioning a mirror. Maybe your previous Cesarean is still a bit unreal, as you never have actually seen a baby leave your body — they tend to just appear from behind the green screen and be held up for a quick look before they disappear to be wrapped up and tested. Make sure that the operating room staff realizes that you would appreciate a verbal description of the birth as it occurs. You may have previously felt left out of your past Cesarean as your body and labor might have been discussed as though you weren’t there. Would you love to meet your new baby in his unclothed, naked newborn state — a wet, slippery baby? Request that the baby be placed on your chest with a warm blanket over you both. It would do a lot to make this surgical delivery a bit more natural for mother, father, and baby. And it may even resolve a few inner conflicts that are faced after the birth. In addition, ask that no screen be placed in the way as you will be able to see the baby as he emerges from your body immediately and even be placed on your chest for the baby checks and to cut the cord. Other options include taking pictures or videotaping the birth, having or even choosing background music to be played during the surgery, and your partner cutting the cord. What about that placenta? Most women who birth vaginally get to see it. If you would like to, too, make sure operating room staff knows you want to view the placenta. Make sure they realize the importance of this, and let them know not to just discard a part of you that you have carried for nine months as insignificant. You may like to take the placenta home, to plant under a tree, or even to eat (it reduces the incidence of postpartum depression), so please tell them to be sure to make suitable arrangements with you to see that this happens. If an emergency Cesarean is necessary, under general anesthetic, then you can have your baby given to your partner as soon as possible after birth and held by him (hopefully next to his naked chest – skin-to-skin contact) until you are awake and can be told of the baby’s sex and well-being by your partner. As with any surgery, there are risks and sometimes those risks can have drastic consequences. Some obstetricians remove the uterus to solve a problem like hemorrhage. Is this a concern for you? Many times, a hysterectomy can be avoided using other treatments. Have you considered the option of tubal ligation during the surgery? Many women have been asked on the operating table this question and have answered hastily only to regret it later. Make the decision before your surgery. Also, with any surgery, administration of blood products may be an option when there is excessive bleeding. Many have fears or religious considerations surrounding the dispensation of blood and blood products. Options may include banking your own blood or refusing blood products and building your own supply back to normal in the days following your birth. Finally, there are two methods to closing the uterus. Highly recommended is the double suturing method (suturing of both the inner wall and outer layer of the uterus) to further ensure scar integrity for subsequent pregnancies and labors. Closure of the skin layer can be done either with staples or with sutures. If either of these is preferable, note it on your birth plan as well.
Example:
I do not consent to having my arms strapped down unless I am physically unable to control them. I am familiar with surgical fields and understand the necessity of maintaining a sterile surgical field.
- Infant Care — How about breastfeeding your baby straight away, rather than hours later? Let them know that you would like to feed your baby while you are being sutured, if you feel up to it, and you would like your baby to stay with you throughout the surgery and even during the recovery. Your baby should remain with you at all times, no disappearing off to the nursery with your partner. This simple routine can seriously affect your bonding with your child. If your baby must go to the nursery, then do send your partner and encourage skin-to-skin contact. Your baby will be much less stressed when with someone he recognizes, as baby will respond to your partner’s voice. Let them know that your partner would be delighted to hold his child within your view throughout these procedures, if you feel unable to participate in the bonding. Newborns are also subjected to various interventions, too — routine health checks using the APGAR assessment, vitamin K injection, eye ointment application, PKU test, weight and height measurements, a bath, and possibly Hepatitis B or other vaccinations. It is highly recommended you research each of these and make an informed decision on allowing, delaying, or not allowing these procedures. You can also ask that the procedures that are done right after baby’s birth be done while in your presence rather than in the nursery. If you are planning to breastfeed your baby, you may want to include in your birth plan that you would like your baby to avoid artificial nipples or supplements including water, sugar water, or formula. If there is a glucose or nutritional concern, ask that it be discussed with you before an action is taken.
Example:
We do not consent to the PKU test until after my milk is in. We believe that this will reduce the likelihood of an inadequate sample, making it less likely a retest will be needed.
Discuss this topic with other API members and parents. Get advice for your parenting challenges, and share your tips with others on the API Forum.
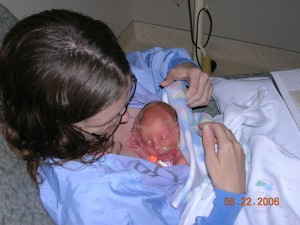 We now have a multitude of studies that show mothers and babies should be together, skin-to-skin (baby naked, not wrapped in a blanket), the baby’s neck extended slightly so his head is in “sniffing position,” immediately after birth – and they should spend as much time together skin-to-skin as possible in the days that follow. The baby is happier, the baby’s temperature is more stable and more normal, the baby’s heart and breathing rates are more stable and normal, and the baby’s blood sugar levels are better.
We now have a multitude of studies that show mothers and babies should be together, skin-to-skin (baby naked, not wrapped in a blanket), the baby’s neck extended slightly so his head is in “sniffing position,” immediately after birth – and they should spend as much time together skin-to-skin as possible in the days that follow. The baby is happier, the baby’s temperature is more stable and more normal, the baby’s heart and breathing rates are more stable and normal, and the baby’s blood sugar levels are better. In preparing the Spring 2009 issue of The Attached Family, I asked a number of women to tell their birth stories who were too uncomfortable in doing so. They were still working through emotions of disappointment, fear, and sometimes guilt surrounding their baby’s birth – even years afterward.
In preparing the Spring 2009 issue of The Attached Family, I asked a number of women to tell their birth stories who were too uncomfortable in doing so. They were still working through emotions of disappointment, fear, and sometimes guilt surrounding their baby’s birth – even years afterward.